Accelerating Quality and Efficiency: A QA Transformation Journey for a Leading Health Plan
Home » Payer
Challenge
A prominent health plan serving millions of members faced multiple, interrelated challenges that were impacting its efficiency and profitability. Key among these was a lengthy end-to-end (E2E) and user acceptance testing (UAT) cycle that extended up to eight weeks per release. This drawn-out testing period meant the health plan could only manage three production releases per year, severely limiting their ability to roll out new features and improvements at a competitive pace. Compounding this issue, their automation coverage was only 25%, leaving most testing processes manual and time intensive. Consequently, approximately 12% of defects were only identified post-deployment, resulting in costly fixes, potential disruptions in service, and a negative impact on the user experience.
Recognizing the need for a strategic transformation in their quality assurance (QA) approach, the health plan partnered with Emids to overhaul their QA processes, aiming to streamline testing, increase automation, and improve release frequency without compromising quality.
Solution
Emids implemented a robust QA transformation program designed to address these specific challenges and create a scalable, high-quality QA ecosystem. The transformation was grounded in a deep understanding of the client’s unique testing requirements and was executed through several targeted strategies.
QA Best Practices & Quality Tracking
Emids established and enforced stringent QA standards to ensure consistency across all testing phases. These best practices created a foundation for thorough quality tracking, allowing the health plan to monitor the effectiveness of their QA processes at each stage. With these standards in place, Emids was able to increase the reliability and quality of every release.
Automated Backlog Management
Emids deployed a centralized team focused on identifying and prioritizing backlogged tasks for automation, enabling the health plan to address pending issues and eliminate bottlenecks more effectively. By reducing manual effort, the team helped streamline the testing workflow, making the process faster and more efficient.
Automated Execution and Testing
Emids committed to significantly increasing automation coverage within the QA process, ensuring that all core functionalities and new features underwent automated testing before release. This automation framework guaranteed consistency in testing, reduced human error, and minimized manual interventions, enhancing both the speed and accuracy of the testing process. This approach not only accelerated release cycles, but also delivered high-quality, reliable products to market with each deployment.
Data Obfuscation for Security and Compliance
To safeguard sensitive member information, Emids implemented advanced data obfuscation techniques, anonymizing production data used in development and QA environments. This step significantly reduced the risk of data exposure, ensuring that all testing adhered to industry standards for data security and compliance.
Self-Service Test Data Generation
Emids introduced a self-service utility that allowed QA teams and developers to generate test data on demand. This tool streamlined the testing process by empowering teams to quickly access the data they needed without dependencies, resulting in enhanced operational efficiency and effectiveness.
Outcome
The QA transformation initiative delivered measurable, impactful results for the health plan, substantially improving both operational efficiency and product quality. The following key outcomes demonstrate the impact of the initiative.
Faster Time to Market
By reducing the end-to-end testing duration by 25%, Emids enabled the health plan to accelerate its release cycle. This reduction allowed the health plan to introduce two additional production releases annually, improving their competitive positioning and responsiveness to market demands.
Increased Efficiency and Defect Reduction
With enhanced QA processes and increased automation coverage, the defect rate in production was significantly reduced. Late defect identification dropped by 70%, resulting in fewer post-deployment issues and improved product reliability. This reduction in defects also led to enhanced user satisfaction and decreased maintenance costs.
Enhanced Automation Coverage
Automation coverage rose dramatically, reaching 75% of the testing processes. This was achieved through the development of a more robust automation framework, featuring reusable components that improved productivity and efficiency by 40%. As a result, the health plan benefited from faster, more reliable, and more scalable QA processes.
Through this QA transformation, Emids empowered the health plan to deliver high-quality products more efficiently and with greater speed. The strategic improvements in quality assurance processes provided the client with a scalable solution that supported rapid growth, reduced operational risks, and positioned them for long-term success in a dynamic healthcare market.
Learn how Payers with the right approach of Quality Engineering can drive sustainable cost optimization for their business.
Transforming Operations with Intelligent Automation for a Leading Health Plan
Home » Payer
Challenge
A leading health plan with millions of members faced significant operational inefficiencies due to manual processes across multiple departments. These inefficiencies were time-consuming, hindered service quality, and negatively impacted the organization’s bottom line. Key areas such as Claims, Care Management, Enrollment & Billing, and Pharmacy Benefit Management were experiencing bottlenecks, leading to delays, higher operational costs, and reduced productivity. The health plan recognized the need to streamline operations through automation to boost productivity and improve cost-effectiveness.
Solution
The health plan partnered with Emids to deploy an enterprise-wide intelligent automation solution. Leveraging UiPath’s automation platform, Emids implemented a comprehensive suite of automated processes across multiple business functions. The solution included:
- Automation Center of Excellence (COE) Setup: Emids established an Automation Center of Excellence (COE) to identify high-impact automation use cases and ensure alignment with the health plan’s business objectives. This COE developed a long-term automation roadmap, ensuring the successful deployment of automation across the organization.
- Intelligent Process Automation Strategy and Roadmap: A comprehensive automation strategy was created to prioritize and streamline processes across departments. This roadmap served as a guide for automating various business functions and driving continuous improvements.
- Automation of Key Business Processes: Emids automated critical processes in areas such as:
- Claims Processing
- Care Management
- Enrolment & Billing
- Pharmacy Benefit Management
- Customer Service and Appeals
These automations significantly reduced manual efforts and increased operational efficiency across the board.
- Savings Dashboard: A customized savings dashboard was implemented to provide real-time tracking of the financial and operational impacts of automation. This allowed the leadership to monitor performance and adjust strategies based on data-driven insights.
Outcomes
The implementation of intelligent automation delivered significant results for the health plan, leading to improved productivity, cost savings, and operational efficiency. Key outcomes included:
- 650,000+ hours saved across the organization through process automation.
- 370+ processes automated across claims, billing, and enrolment.
- Cumulative savings of over $12M within the first three years, delivering a 400% ROI.
- 14,000 COVID-related claims adjustments processed within three weeks, showcasing the agility and responsiveness of the automation system.
- 40% reduction in processing time for primary care provider (PCP) change requests.
- More than 30% reduction in clinicians’ administrative tasks, allowing for more time to focus on patient care.
- $600K savings from the automation of the claims process alone.
- Real-time reporting of bot performance, providing operational insights and enabling continuous refinement of the automation strategy.
By integrating intelligent automation into their core processes, the client achieved significant operational efficiencies, cost savings, and service improvements. The success of this initiative positioned them to leverage automation as a key component of its long-term strategy, ensuring a competitive edge in the healthcare industry.
Explore how Payers can unlock sustainable cost optimization by enhancing their operational efficiency.
From On-Prem to Google Cloud for a leading US Healthcare Player
Home » Payer
Challenge
A prominent healthcare organization in the USA, managing diverse business lines including retail, pharmacy, health insurance, managed healthcare, and population health management, sought to modernize its data ecosystem. The goal was to transition from on-prem systems to the Google Cloud Platform (GCP) to leverage the full potential of their data, enhance scalability, and streamline operations. However, the cloud migration posed significant challenges, such as handling large datasets, ensuring data integrity, and maintaining uninterrupted business operations during the transition.
Solution
Emids executed a well-orchestrated, multi-phase migration plan. The journey began with meticulous planning, involving comprehensive collection of details about the client’s workloads, schemas, users, and source systems. This exhaustive analysis was crucial in crafting a tailored migration strategy for a smooth transition.
Migration Planning: Detailed information on workloads, schemas, users, and source systems was collected, forming the basis for a customized migration strategy.
Schema Design and Data Rationalization: The target schema was designed and data sets were rationalized to optimize performance and scalability on GCP.
Data Migration: Data was migrated from Hadoop to BigQuery, encompassing both one-time data transfers and the setup of incremental workload processes. This included data replication, transformation, and ingestion to ensure efficient and accurate data movement.
Workload and Application Migration: The migration of workloads and applications was managed by converting code from HQL to BigQuery SQL and adapting scripts using Python and PySpark. Airflow was utilized for job scheduling and monitoring to ensure seamless and continuous operations.
Application Management and Validation: Robust application management tools were set up, including cost monitoring with Apptio and application monitoring with New Relic. Extensive data validation, end-to-end testing, and a production parallel run were conducted to ensure system reliability.
Decommissioning and User Adoption: The Hadoop environment was decommissioned, on-prem data removed, scheduled jobs terminated, and end-user adoption of the new system facilitated.
YOUR PARTNER IN CLOUD TRANSFORMATION
Advanced Cloud Migration Solutions
Expert-led cloud migration services designed to optimize costs, enhance innovation, and mitigate risks for healthcare organizations.
Discover our Cloud Migration Solutions
Outcome
The project delivered transformative results for the healthcare organization:
Successful Migration: The healthcare business unit’s data was seamlessly migrated to GCP, establishing a new semantic layer that improved data accessibility and usability.
Enhanced Data Processing: The new cloud infrastructure provided enhanced data processing capabilities, supporting a broader range of use cases and enabling rapid scaling to meet business demands.
Operational Excellence and Cost Management: With modern tools and optimized processes, the organization experienced improved operational efficiency, reduced costs, and better data management. The cloud environment facilitated advanced analytics and business insights, driving growth and innovation.
Cloud Migration and CMS Interoperability for a Leading HMO
Home » Payer
Challenge
A non-profit Health Maintenance Organization (HMO), wanted to modernize its IT ecosystem. This included a crucial migration to the cloud, constructing next-generation data platforms, and upskilling their workforce to support their growth trajectory. They were also driven by the need to comply with the Centers for Medicare & Medicaid Services (CMS) Interoperability and Patient Access final rule, which mandates that patients have access to their health information through standardized APIs like HL7 FHIR. The HMO faced significant challenges in ensuring seamless data migration while adhering to stringent compliance requirements and modernizing their infrastructure.
Solution
Emids was brought in to navigate these complex requirements and provide a robust solution. We began by developing a comprehensive cloud strategy that encompassed a detailed data platform strategy on AWS.
Our approach was multifaceted:
Leverage CMS Interoperability Program: Using the CMS Interoperability program as a minimum viable product, we ensured that our solution met immediate compliance needs while setting the foundation for future expansion.
Data Mapping and Architecture: We meticulously mapped data from the HMO’s source systems to the FHIR store, ensuring accuracy and completeness. Our team designed an architecture pattern tailored to the client’s needs, establishing AWS infrastructure and CI/CD pipelines for streamlined operations.
Data Migration: Utilizing tools like Sqoop, we migrated data from on-prem databases to AWS S3 buckets. We then implemented a FHIR server, converting data into the FHIR format and loading historical data into an MS SQL Server in FHIR format.
Data Pipelines and Authentication: We created data pipelines using AWS Glue, Python, and Lambda to handle incremental data loads from new systems to the cloud. Additionally, we enabled member authentication and authorization using Okta, ensuring secure access to data.
YOUR PARTNER IN CLOUD TRANSFORMATION
Advanced Cloud Migration Solutions
Expert-led cloud migration services designed to optimize costs, enhance innovation, and mitigate risks for healthcare organizations.
Discover our Cloud Migration Solutions
Outcome
The project was executed with precision, leading to several significant outcomes:
Architectural Excellence: We delivered a robust cloud architecture pattern that provided a scalable and efficient framework for the HMO’s operations.
Enhanced Compliance and Interoperability: The HMO achieved full compliance with CMS mandates, providing patients with seamless access to their health information via FHIR APIs. This not only met regulatory requirements but also enhanced internal data exchange processes.
Operational Efficiency: Data on the cloud facilitated advanced analytics, improving decision-making and operational efficiency. The new system supported rapid data access and processing, empowering the HMO to offer better services to its members.
Transforming IT Infrastructure for a Top-Tier Healthcare Company
Home » Payer
One of the largest healthcare companies in the Fortune 500 approached Emids with a vision for a modern IT ecosystem. They found themselves in a situation where their IT infrastructure and capabilities were not scalable to support their rapid growth.
These infrastructural shortcomings were not merely internal roadblocks. They directly impacted the customer experience and created friction between different businesses within the enterprise.
The customer wanted to build an IT ecosystem that would enable swift integration of its various lines of businesses from a data perspective and place them on a scalable, secure, and flexible cloud platform.
The goal was to develop an enterprise platform that supported the organization’s future organic and inorganic growth endeavors, and that also leveraged its current assets. To realize this vision, the client required a strategic partner with extensive experience in strategic consulting, data & digital engineering, and product engineering.
Emids was brought in to provide technical leadership while building a cloud data platform and various enterprise data products. Emids also supported the building of enterprise governance processes along the way to ensure data was being accessed, processed and stored in line with organizational policies.
The solution involved a three-pronged approach:
- Operating Model Development: Emids designed an Operating Model for a multi-tenant ecosystem grounded in four principles: Minimum friction across all interactions, Self-Service, Tenant Collaboration, and Risk Reduction. This model served as a blueprint, outlining the organization’s data-focused operations, enabling them to manage, share, and utilize data for insights and business outcomes.
- Data Strategy Formulation: Emids collaboratively developed a data strategy with various lines of businesses, enabling subsidiaries to use data in a self-serve manner while migrating existing data to the enterprise platform. This alignment of data strategy with the corporate vision ensured a unified data-driven culture across the organization.
- Enhancement of Platform Capabilities: Emids defined and prioritized platform capabilities such as DevOps patterns, infrastructure automation, test data management, data catalog, and metadata management. These capabilities empowered internal teams to build new solutions effectively and manage data efficiently.
Thanks to its deep domain expertise and outcome-oriented team, Emids delivered a modern IT ecosystem including a robust data platform to support the organization’s overall growth and collaboration among lines of businesses. The scalable and secure IT ecosystem now stands ready to support the client’s growth vision.
Enterprise Data Platform Implementation for Leading Payer
Home » Payer
The Emids customer is a leading payer—with nearly 47 million members operating across the commercial, Medicare, and Medicaid markets—focusing on whole-person health for improving outcomes.
The customer had developed and acquired applications across their business, primarily leveraged for internal use with a few external clients. They saw a market opportunity to commercialize these apps for external use. The key challenge was that the suite of applications wasn’t created for data ingestion from external sources. Emids was approached to build an ingestion framework that allowed for these apps to absorb data from both internal and external sources.
Having a tight deadline of six months, the customer tasked Emids with developing a cloud-data platform with the ability to ingest data from multiple parties in a secure, multi-tenant way. That’s where Emids’ CoreLAKE™ came into the picture.
CoreLAKE™ is a ready-to-implement data management solution that can ingest and integrate disparate data in a comprehensive health care data model—helping customers get to market faster.
The customer’s data platform was built on CoreLAKE™ and deployed on the Google Cloud Platform to ingest, cleanse, standardize, and harmonize the data streams coming from multiple external sources into a unified data model residing in Snowflake.
Emids helped the customer integrate with their existing client systems and provided high-quality data delivery via CoreLAKE™, which also enabled the client to build upon their high-value analytics assets. Emids also provided end-to-end data operations to achieve significant cost reduction.
Through its deep domain & technical expertise, Emids helped accelerate the client’s time to value using CoreLAKE™’s out-of-the-box functionalities.
Data Engineering
Make Data Your Business Advantage
Emids can help you manage and effectively use data for optimal results. We have a process-oriented approach to data management, consisting of data stewardship, data quality, data security and metadata management.
Learn More
Humana’s Low-Code Partnership Approach to Rapid Digital Innovation
Home » Payer
In an era of rapid digital healthcare innovation, Humana, the third largest health insurance company in the U.S. faced several challenges within its digital channels unit to rapidly bring new solutions to market. It was laden with complex architecture, which meant IT had to tread carefully, given the importance of safeguarding personal health information for millions of members.
Amid this complexity and the COVID-19 pandemic, Humana needed a solution for its contact center’s number one ask: locating a COVID-19 testing center for its members.
The existing giant spreadsheet was slowing down contact center staff, so Humana turned to its low-code delivery partner, Cloud Development Resources (CDR)—an Emids company—to co-deliver a solution on the OutSystems platform. Through this low-code co-creation approach, Humana was able to create the web app experience on OutSystems in a weekend and Emids was brought in to develop a full suite of back-office functions, allowing 30 reps to regularly update the testing locations database in real time on the web app.
Within a month, Emids also created a mobile-friendly customer-facing app to help members directly find testing sites through a Google-map-like search experience leveraging artificial intelligence in OutSystems.
Speed to market is a key challenge for digital innovation and Humana now delivers four times faster for its members thanks to a low-code platform approach to application development and its partnership with CDR. This shows that a vast range of innovations once considered cost-prohibitive or risky are now viable. Finally, Humana now has a mobile-friendly customer-facing app that allows members to self-serve, taking pressure off of their call center agents.
Emids Low-Code
Accelerated Web and Mobile Development
The Emids low-code solutions practice leverages a deep bench of experienced problem solvers to help you craft enterprise-grade applications, providing trusted advice as we seek new ways to amplify results.
Learn More
Learn more about the partnership between CDR, OutSystems and Humana here.
Experience Design of a Direct-to-Consumer Care Portal
Home » Payer
Emids worked with a top Fortune 500 payer organization, which aims to empower their over 100m members to live healthier lives.
The organization wanted to complement its care advisors with a high touch, digital concierge experience for families experiencing complex care needs regardless of their health plans. The objective was to free up space for the provider and specialty-care practices so they could focus on care delivery and member health.
Selected for its deep healthcare domain and user-centered design expertise, Emids took a deep dive into the portal’s existing experience and also assessed user challenges through a month-long discovery session.
Throughout the discovery process, Emids focused on the journeys of prioritized users to identify opportunities for delivering a better user experience. Emids created user scenarios and flows to describe an ideal experience from the users’ perspective and prepared necessary UX requirements and recommendations to support future product development efforts.
EMIDS DESIGN LED PRODUCT ENGINEERING
Create a Path for Consumer Experience Success
See how Emids takes a design-led approach to product development.
Learn More
Through continued collaboration with the client team, Emids delivered a UX Playbook to serve as a reference point for product decisions going forward, including research findings and recommendations and design decisions. Emids also delivered two prototypes to reference for the MVP and Beyond the MVP work, highlighting key service design considerations as the project continues into the build phase.
Compliance with CMS Interoperability & Patient Access Final Rule
Home » Payer
Overview
The Emids client is a not-for-profit 501c3 health maintenance organization (HMO) insurance company with a consistent record of earning accreditation by the National Committee for Quality Assurance (NCQA).
Emids partnered to help them build the right capabilities that comply with Centers for Medicare and Medicaid (CMS) regulatory requirements related to Interoperability and Patient Access final rules. These regulatory requirements are applicable to the client’s LOBs – Medicaid and Duals only.
The Challenge
Developing interoperability preparedness for not only regulatory compliance but “beyond the rules” readiness.
Emids Solution
Our team performed a discovery assessment to understand as-is state and data ingestion process, data flows, technology and integration tools. We carried out a detailed assessment around FHIR integration, “Build on Cloud” solution approach, and discovered FHIR resource gaps within the current data landscape.
Based on our analysis, we explored multiple options to comply with the CMS Interoperability mandate, developed a future state architectural blueprint, identified selective use cases related to regulatory mandates and created a detailed implementation road map, including an overall operating model.
Our team implemented a selected interoperability solution option including cloud infrastructure setup, building authentication and authorization mechanism using OKTA, implementing an FHIR server for exchange as well as storage of healthcare data exchange and exposing data using FHIR compliant APIs. This solution approach was forward-thinking to anticipate and build new member engagement and data analytics capabilities down the line.
DATA ENGINEERING
Make Data Your Business Advantage
See how Emids can help you manage and effectively use data for optimal results.
Learn More
Results
In 10 months we helped the client meet the Patient Access API & Provider Directory API deadline of CMS mandate.
Enhancing the Overpayment Recovery Process to Result in Savings
Home » Payer
Overview
The Emids client is a pharmacy benefit manager and care services group with over $100 billion in revenue. They have three main businesses, all of which strive to deliver transformational healthcare solutions and improve outcomes while lowering costs. We have partnered with the client for over 10 years, during which time they have provided data mining and overpayment recovery services for physicians and facility claims for three specific lines of business – employer and individual, Medicare and retirement and administrative services.
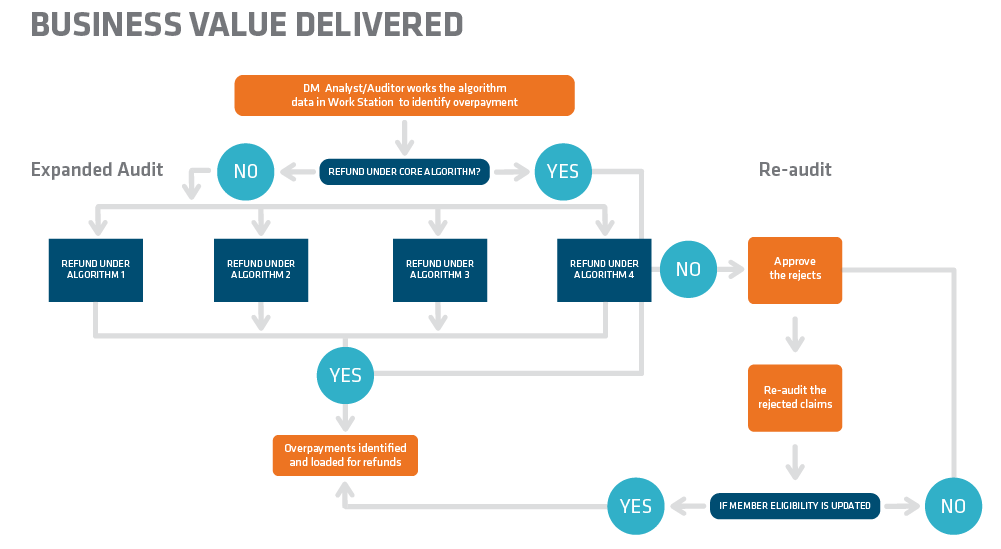
Our team had been auditing all client-paid claims to providers using various algorithms and business rules as a part of the overpayment recovery process. For the algorithms coordination of benefits (COB) and member’s eligibility/coverage-related (Retro Term), auditors used consumer database (CDB) – a Web-based application – as the source for accurate coverage data and relied on the information available at the time of the audit. CDB was updated whenever a change in information occurred, such as new member coverage. The client then provided a member analysis report in which external vendors identified the overpaid claims that were initially rejected (considered paid correctly) by our auditors, based on the information stated in the CDB.
For each overpaid claim identified by an external vendor, the client was paying a premium which led to revenue loss.
Solution
Our team analyzed the situation and realized that if all rejected claims from COB and Retro Term were re-audited with a lookback period, an opportunity existed to identify overpayment for those specific claims in which member information was updated after our audit, and before the external vendor began identifying the rejected claims.
They subsequently tweaked the current process by introducing a re-audit, during which COB and Retro Term rejected claims were reviewed with a lookback period of two months, considered the standard timeframe to upload the member’s updated coverage information in CDB. Also taken into account was the standard lag time for the external vendor to begin identifying the rejected claims. Based on past data analysis, our team identified that claims valued at more than $5k, which comprised 2% of the total inventory covering 45% of the total claims value, could be re-audited to reduce the revenue leakage.
Our project team members were trained in COB and Retro Term algorithms and given access to all required applications to complete the re-audit.
Results
By introducing a re-audit of the overpayment recovery process, our team has saved the client $885k to date without impacting productivity, turnaround time and quality metrics.
Contact us to learn more about partnering opportunities.