Overview
The Emids client is a pharmacy benefit manager and care services group with over $100 billion in revenue. They have three main businesses, all of which strive to deliver transformational healthcare solutions and improve outcomes while lowering costs. We have partnered with the client for over 10 years, during which time they have provided data mining and overpayment recovery services for physicians and facility claims for three specific lines of business – employer and individual, Medicare and retirement and administrative services.
Our team had been auditing all client-paid claims to providers using various algorithms and business rules as a part of the overpayment recovery process. For the algorithms coordination of benefits (COB) and member’s eligibility/coverage-related (Retro Term), auditors used consumer database (CDB) – a Web-based application – as the source for accurate coverage data and relied on the information available at the time of the audit. CDB was updated whenever a change in information occurred, such as new member coverage. The client then provided a member analysis report in which external vendors identified the overpaid claims that were initially rejected (considered paid correctly) by our auditors, based on the information stated in the CDB.
For each overpaid claim identified by an external vendor, the client was paying a premium which led to revenue loss.
Solution
Our team analyzed the situation and realized that if all rejected claims from COB and Retro Term were re-audited with a lookback period, an opportunity existed to identify overpayment for those specific claims in which member information was updated after our audit, and before the external vendor began identifying the rejected claims.
They subsequently tweaked the current process by introducing a re-audit, during which COB and Retro Term rejected claims were reviewed with a lookback period of two months, considered the standard timeframe to upload the member’s updated coverage information in CDB. Also taken into account was the standard lag time for the external vendor to begin identifying the rejected claims. Based on past data analysis, our team identified that claims valued at more than $5k, which comprised 2% of the total inventory covering 45% of the total claims value, could be re-audited to reduce the revenue leakage.
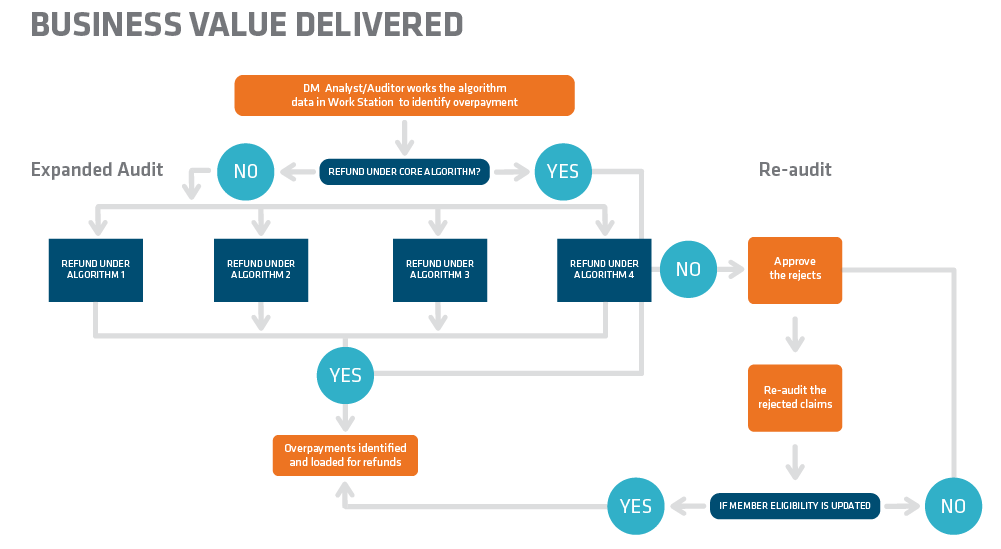
Our project team members were trained in COB and Retro Term algorithms and given access to all required applications to complete the re-audit.
Results
By introducing a re-audit of the overpayment recovery process, our team has saved the client $885k to date without impacting productivity, turnaround time and quality metrics.
Contact us to learn more about partnering opportunities.