How the right data governance model can help healthcare organizations meet the demands of digital transformation
By Randy Thomas, FHIMSS
Senior Director, Value-based Consulting
Value-based care. Population health management. Digital health. Healthcare consumerism. Promoting interoperability. All these evolving healthcare opportunities require consistent, accurate, reliable data. While the quantity of data created in healthcare continues to grow–fueled by the ubiquitous adoption of EHRs–many organizations do not yet have a pragmatic, robust, enterprise-wide approach to ensuring their data is “in shape.” This is where data governance enters the scene.
Organizations must be confident that the data used to provide patient care, improve performance, negotiate contracts and inform decision-making across the organization is reliable and accurate. Data governance provides the structure and process to ensure the needed reliability and accuracy to promote interoperability and data exchange.
Data needs to be appropriately used and accurate for its purpose, and it should also flow quickly and easily for optimum use (i.e., is “liquid”). The data chain of trust flowing from source to target needs to be clear and well documented, so the resulting integrated view can be considered reliable to support reporting, measurement and analytics. Enabling this data liquidity requires hands-on governance to establish and maintain data sources, definitions and uses.
A cross-functional data governance structure and process can help organizations create that chain of trust and harness the value of their data assets. But be aware—data governance is not an information technology (IT) function nor is it a department in the organizational hierarchy. Rather, data governance brings together the key stakeholders from quality, finance, administration, IT and others to make decisions on how data should be captured, standardized, used and secured.
The data governance discipline is responsible for maintaining documentation, by data element, of which systems capture the data. It makes decisions on how to rationalize inconsistencies in data that is allegedly the same. It governs how the data can be used to ensure appropriate access, security and patient privacy. And if necessary data is not captured in the way that is usable (or not captured at all), it identifies the need for potential changes in workflow and system implementation and engages the right stakeholders to effect the required modifications.
Even though the purpose of data governance is always the same, the formal structure of each data governance implementation should be aligned with each organization’s guiding principles, decision, style and culture.
The complex and diverse environment of most healthcare organizations necessitates a multi-tiered, multi-discipline approach to a governance structure regardless of which model is selected. A standing, hierarchical governance model that governs data as well as business intelligence activities is often the preferred alternative.
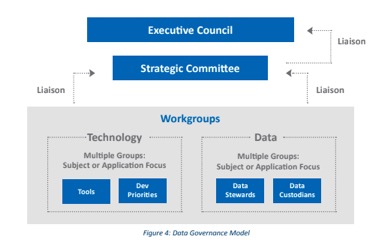
This structure appropriately distributes the decision-making and provides the opportunity for broad participation across an organization. Frequently, existing governance groups can be leveraged to help ensure participation and avoid increased meeting burden on executives.
When initializing a data governance process, organizations should focus on a specific issue–such as understanding the data that underlies the quality measures used in value-based contracting. Identifying and defining this initial data set adds immediate value (i.e., ensuring accurate metrics) and establishes the foundation of data governance practices that can scale to encompass additional areas of focus, additional data sets.
Data is a valuable enterprise asset. Accurate data doesn’t just happen. It’s the result of a pragmatic data governance program with enterprise-wide participation.
To learn more about the right data governance strategy and model for your organization, download our latest white paper, “The Importance of Data Governance in Value-based Care.”

