Enhancing the Overpayment Recovery Process to Result in Savings
Overview
The Emids client is a pharmacy benefit manager and care services group with over $100 billion in revenue. They have three main businesses, all of which strive to deliver transformational healthcare solutions and improve outcomes while lowering costs. We have partnered with the client for over 10 years, during which time they have provided data mining and overpayment recovery services for physicians and facility claims for three specific lines of business – employer and individual, Medicare and retirement and administrative services.
Our team had been auditing all client-paid claims to providers using various algorithms and business rules as a part of the overpayment recovery process. For the algorithms coordination of benefits (COB) and member’s eligibility/coverage-related (Retro Term), auditors used consumer database (CDB) – a Web-based application – as the source for accurate coverage data and relied on the information available at the time of the audit. CDB was updated whenever a change in information occurred, such as new member coverage. The client then provided a member analysis report in which external vendors identified the overpaid claims that were initially rejected (considered paid correctly) by our auditors, based on the information stated in the CDB.
For each overpaid claim identified by an external vendor, the client was paying a premium which led to revenue loss.
Solution
Our team analyzed the situation and realized that if all rejected claims from COB and Retro Term were re-audited with a lookback period, an opportunity existed to identify overpayment for those specific claims in which member information was updated after our audit, and before the external vendor began identifying the rejected claims.
They subsequently tweaked the current process by introducing a re-audit, during which COB and Retro Term rejected claims were reviewed with a lookback period of two months, considered the standard timeframe to upload the member’s updated coverage information in CDB. Also taken into account was the standard lag time for the external vendor to begin identifying the rejected claims. Based on past data analysis, our team identified that claims valued at more than $5k, which comprised 2% of the total inventory covering 45% of the total claims value, could be re-audited to reduce the revenue leakage.
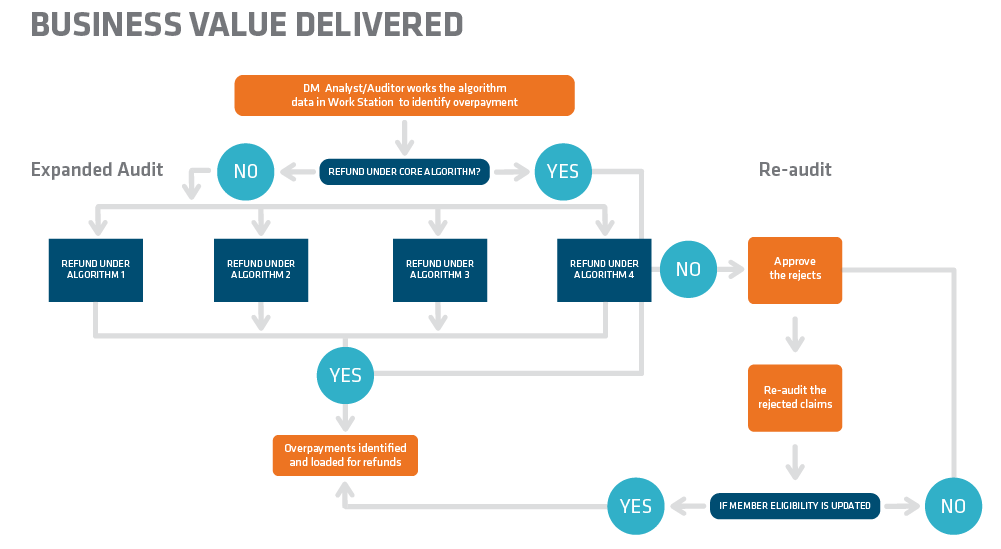
Our project team members were trained in COB and Retro Term algorithms and given access to all required applications to complete the re-audit.
Results
By introducing a re-audit of the overpayment recovery process, our team has saved the client $885k to date without impacting productivity, turnaround time and quality metrics.
Contact us to learn more about partnering opportunities.
How a Health System Implemented a Population Health Platform for Medicaid Program
emids delivered project management, change management and training services to help UHS care managers meet new state requirements.
Overview
United Health Services (UHS) is an upstate New York integrated health system comprised of four hospitals, a senior residence, physician practices and a home health organization.
In 2016, the organization now had to comply with the New York State Medicaid Health Home (MHH) program. This included automating the care management workflows to support the health home processes. New York’s health home requirements included data integration with a regional health information exchange (HIE). Noncompliance would jeopardize UHS’ Medicaid reimbursement. We facilitated a vendor evaluation and selection process which identified Netsmart as the vendor of choice. We also worked closely with Netsmart and UHS to complete the pre-implementation planning work in a rapid timeframe, in preparation for the aggressive implementation schedule.
Solution
The implementation of Netsmart’s care coordination application began in June 2017, giving UHS less than four months to have the system ready for care managers in time for the state’s Medicaid deadline. Due to the tight timelines and the critical nature of the project, UHS care management and IT leaders knew strong change management support would be needed. We had proven experience successfully leading care management toolset implementations with change management support for large healthcare organizations, making us an excellent fit for this high-stakes project.
We applied proven processes to coordinate between the UHS care management team, the vendor and the regional HIE. This provided integrated project management, communication, risk management, quality assurance and data validation, training, and support throughout the four-month implementation.
Results
We supported the growth of UHS’ MHH program, ensuring the state’s requirements and deadline were met.
“The team at emids did a wonderful job of understanding and accounting for our organizational culture, creating smooth change management and transition plans for our staff,” said Annie DePugh, director of population health at UHS. “We were thrilled to maintain an on-time delivery schedule and avoid issues that could have been a roadblock with our care managers.”
Healthcare providers must continuously stay on track with changes in federal reimbursement programs, which often call for new IT requirements and workflow modifications. Complexities often come up when transitioning to new workflows and toolsets. We were a key partner in helping UHS evolve rapidly to meet an important new set of Medicaid Health Home requirements, ensuring consistent program operations and the best possible care for its chronic Medicaid population.
How a Health System Selected a Population Health Platform for Medicaid Program
emids helped a large healthcare organization select a new vendor and plan the implementation to meet New York State Medicaid requirements.
Overview
United Health Services (UHS) is an upstate New York integrated health system comprised of four hospitals, a senior residence, physician practices and a home health organization.
In 2016, the organization was in a pressing position to comply with New York Medicaid Health Home (MHH) program changes for managing patients with chronic conditions. UHS needed to implement a care management system to automate the health home processes in a short period of time. The IT requirements included documentation, alerts, reporting, integration and data sharing between an interdisciplinary team of providers and family caregivers. New York’s health home program requirements also included system integration with a regional health information exchange organization, enabling facilities to deliver prompt notification of an individual’s admission and/or discharge from an emergency room, inpatient or rehabilitation setting.
After attempting to select a product and manage a complex implementation, UHS realized some outside guidance and support was needed to meet an aggressive state-mandated deadline.
Solution
UHS came to us for help to find a vendor so they could get the project back on track. The project involved conducting a thorough vendor evaluation and selection process along with the pre-implementation planning work, in a short time frame. UHS selected us for the engagement given our vast knowledge and experience in software selection, planning and implementation. We have developed a methodology to conduct unbiased vendor evaluations and selection, which takes the burden off of clients and saves time. This also helps reduce project risk, as our expertise and approach identifies the best match for an organization’s needs.
The engagement included the following steps and services:
- We documented the requirements and distributed RFQs, followed by a review of vendor responses and a functional, cost, and technical assessment of each product. We also facilitated product demos and conducted reference calls.
- We facilitated a Decision Day, which is a framework we created to guide stakeholders through key project decisions. This framework combines industry experience with the client’s input to form a collaborative approach early on. The result is a process and conclusion that aligns the client priorities and perspectives.
- Once the vendor was selected, we immediately kicked off the pre-implementation planning. This incorporated the creation of an integrated project plan, communication plan, change management plan, risk management plan and training plan.
Results
We helped UHS identify Netsmart as the vendor of choice to meet the New York MHH program requirements. Netsmart began work in mid-June 2017, and the joint team completed the implementation for the state Medicaid program ahead of the Oct. 1 deadline.
“When we had to cancel the original vendor agreement, we were worried about meeting New York’s Medicaid deadlines,” said Annie DePugh, director, population health at UHS. “emids took charge immediately and guided us through a sensible and thorough process for selecting the best possible vendor. The Decision Day framework is a unique and effective way to complete milestones under tight windows.”
Updating systems to meet new industry requirements is always challenging. Our proven methodology for vendor selection and robust project management, change management and training processes helped UHS ensure ongoing Medicaid reimbursement revenue streams.